Symptoms/Signs
- Chest pain
- Hypoxemia
- Tachycardia
- Tachypnea
- Hypotension (if massive, see below)
Wells’ Criteria
- Separate Wells’ criteria for DVT and PE (1)
- Helps risk stratify a patient for likelihood of having a pulmonary embolism based on history and physical exam findings
- Can calculate with an online calculator (i.e. mdcalc.com)
Workup
- CT Angiogram: Gold-standard for diagnosis
- D-Dimer: sensitive, but very non-specific. If ordering this test, must be ready to order a CT angiogram for confirmation if/when it results elevated
- V/Q Scan: A nuclear scan in which radioactive material is inhaled and then administered IV. This gives an image of the ventilation and perfusion ratios of the lungs. This test is mostly useful if pre-test probability is high and and results are strongly suggestive of pulmonary embolism, OR if the pre-test probability is low and the results are strongly suggestive of no pulmonary embolism. This test is sometimes used in order to spare contrast load in a patient with renal dysfunction
- Echocardiography/Point-of-Care Ultrasound (POCUS)
- McConnell’s Sign
- Hypokinesis of the right mid-ventricular free wall with preserved apical systolic motion
- Right ventricular dilation
- McConnell’s Sign
- Lower Extremity Ultrasound and Doppler
- A majority of pulmonary embolisms arise from deep vein thromboses (DVTs) of the lower extremities, so this test may help discover the etiology
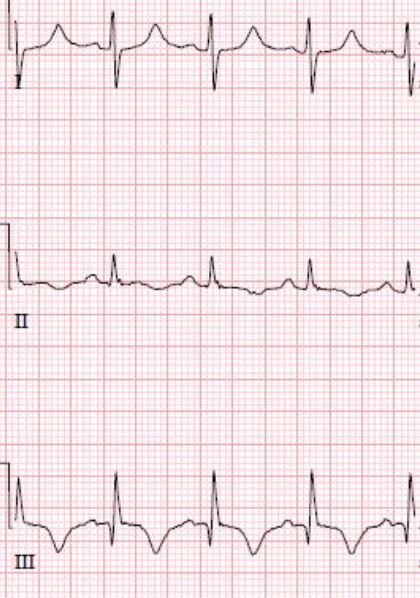
- EKG
- Most common findings: Sinus tachycardia
- Right Bundle Branch Block
- Right Axis Deviation
- S1Q3T3 (S-wave in lead I, Q-waves and T-wave inversion in lead III)
Classification
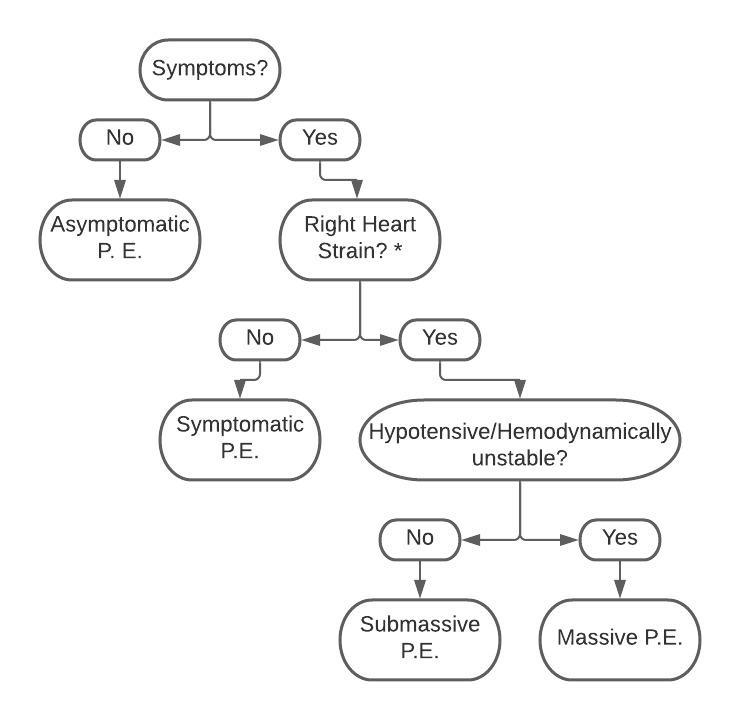
*Right heart strain may be revealed through an elevated BNP or NT-proBNP, elevated troponin, or EKG findings such as S1Q3T3 , right bundle branch block, or right axis deviation. However, the best method of determining right heart strain is from an echocardiogram showing an enlarged right ventricle, as well as potentially showing McConnell’s sign (see above)
Risk Stratification
- PESI: Pulmonary Embolism Severity Index
- Score of 0-350 based on age, gender, medical history, and symptoms/vital signs
- Helps prognosticate patients in terms of 30-day mortality
Management
- Asymptomatic
- Low molecular weight heparin (LMWH), dosed 1 mg/kg BID or continuous unfractionated heparin infusion
- Bridge to warfarin or a direct oral anticoagulant (DOAC) such as direct thrombin inhibitor like dabigatran or factor Xa inhibitor like rivaroxaban
- Symptomatic
- LWMH or continuous unfractionated heparin infusion
- Bridge to warfarin or DOAC
- Submassive
- Continuous unfractionated heparin infusion (this way, if the patient suddenly decompensates, can quickly turn off the infusion and give thrombolytics as below)
- Bridge to warfarin or DOAC
- Massive
- Thrombolysis vs mechanical thrombectomy
- Bridge to continuous unfractionated heparin infusion
- Eventual bridge to warfarin or DOAC
- Duration of therapy
- Transient risk factors: 3 months
- Unprovoked or ongoing risk factors: 6-12 months
References:
- Wells PS;Anderson DR;Rodger M;Stiell I;Dreyer JF;Barnes D;Forgie M;Kovacs G;Ward J;Kovacs MJ;. (n.d.). Excluding pulmonary embolism at the bedside without diagnostic imaging: Management of patients with suspected pulmonary embolism presenting to the emergency department by using a simple clinical model and d-dimer. Retrieved January 14, 2021, from https://pubmed.ncbi.nlm.nih.gov/11453709/

