Shock is defined as circulatory failure resulting in systemic hypoperfusion. Most commonly as a result of low blood pressure.
Approach to the hypotensive patient
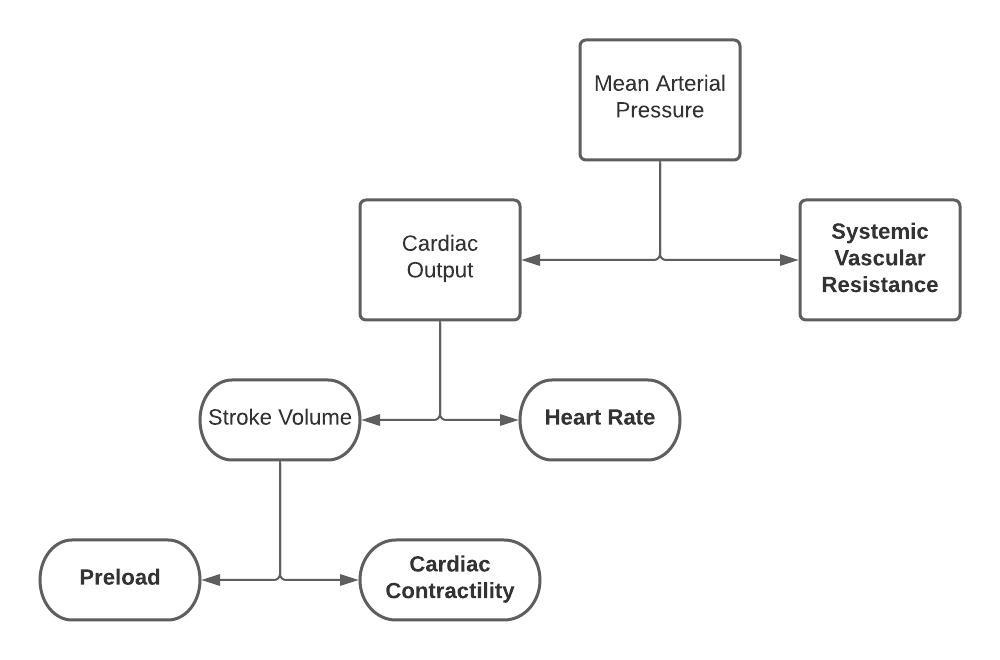
4 factors play a role in hypotension (see figure below)
- Preload
- Cardiac Contractility
- Heart Rate
- Systemic Vascular Resistance
Low Preload
- Poor volume intake
- Treatment: Volume resuscitation
- Volume loss
- Diarrhea
- Diuretics
- Hemorrhage
- Treatment: Volume resuscitation
- Obstruction (inability of blood to get back to Left Atrium)
- Tension Pneumothorax
- Pulmonary Embolism
- Cardiac Tamponade
- Treatment: Volume resuscitation and alleviation of obstruction (needle thoracostomy, fibrinolytic administration, or pericardiocentesis)
- Tachyarrhythmias (inability of the ventricles to properly fill)
- i.e. Atrial Fibrillation with Rapid Ventricular Response, Ventricular Tachycardia, Paroxysmal Supraventricular Tachycardia
- Treatment: Synchronized Cardioversion
Low Cardiac Contractility
- Infarction
- Heart Failure
- Thiamine Deficiency (“wet beriberi”)
- Treatment: Inotropes, ACS management if applicable, high-dose IV thiamine supplementation if suspicious
Low Heart Rate
- Sick Sinus Syndrome
- AV node block (1st degree – 3rd degree)
- Medications (Beta-Blockers, Calcium Channel Blockers)
- Treatment: Atropine followed by transcutaneous pacing
Low Systemic Vascular Resistance
- Sepsis
- Anaphylaxis
- “Neurogenic Shock”: Anesthetics or spinal trauma
- Adrenal Insufficiency
- Liver Failure
- Medications
- Treatment: Vasoconstrictors
- Antibiotics if in sepsis
- IM epinephrine and IV steroids if in anaphylaxis
- Glucocorticoid and mineralocorticoid replacement if in adrenal crisis
- Liver transplant if in liver failure
Evaluation of Shock
Pulse Pressure (SBP – DBP)
- High Pulse Pressure: Think distributive
- Low Pulse Pressure: Think cardiogenic
Extremities
- Warm: Think Distributive
- Cold: Think cardiogenic
Point-of-Care-Ultrasound (POCUS)
- See “POCUS” as its own topic, but in short, can evaluate for volume status, pulmonary embolism, pneumothorax, tamponade, and cardiac function
- Can also assist us in evaluating for fluid responsiveness – can calculate cardiac output as a function of stroke volume before and after fluid administration
Labs
- Lactic Acid
- Elevated in shock due to reversion of cellular metabolism to anaerobic metabolism in the absence of adequate tissue oxygen perfusion
- Can trend as part of evaluation for improved tissue perfusion
- SCVO2 (Central Venous Oxygen Saturation)
- High: Distributive
- Low: Cardiogenic/Hypovolemic
- CVP (Central Venous Pressure)
- High: Cardiogenic
- Low: Distributive/Hypovolemic
- Troponin
- BNP
- EKG
- Infectious workup (blood cultures, urinalysis and culture, chest x-ray)
- AM Cortisol if concerned for adrenal insufficiency